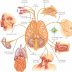
There are 12 pairs of cranial nerves. The names of these nerves are
following.
Ⅰ Olfactory nerve
Ⅱ Optic nerve
Ⅲ Oculomotor nerve
Ⅳ Trochlear nerve
Ⅴ Trigeminal nerve
Ⅵ Abducent nerve
Ⅶ Facial nerve
Ⅷ Vestibulocochlear nerve
Ⅸ Glossopharyngeal nerve
Ⅹ Vagus nerve
Ⅺ Accessory nerve
Ⅻ Hypoglossal nerve
These are classified into sensory, motor and mixed nerves according to their functions.
Sensory cranial nerves: These nerves contain only afferent (sensory) fibers.
They are given below.
Ⅰ Olfactory nerve
Ⅱ Optic nerve
Ⅷ Vestibulocochlear nerve
Motor cranial nerves: These nerves contain only efferent (motor) fibers.
They are given below.
Ⅲ Oculomotor nerve
Ⅳ Trochlear nerve
Ⅵ Abducent nerve
Ⅺ Accessory nerve
Ⅻ Hypoglossal nerve
Mixed nerves: These nerves contain both sensory and motor fibers.
They are given below.
Ⅴ Trigeminal nerve,
Ⅶ Facial nerve,
Ⅸ Glossopharyngeal nerve
Ⅹ Vagus nerve
- Olfactory nerve (first cranial)
It is
purely sensory nerve. The sensory receptors of the olfactory nerve are located in the
superior nasal conchae (ethmoid bone) of the nose. The
olfactory filament arises from the sensory receptors which pass through the
foramina in the cribriform plate of the ethmoid bone. The olfactory filament ends at the
olfactory bulb which lies just above the cribriform plate. Olfactory bulb continues posteriorly as the
olfactory tract. Olfactory tract ends at the floor of cerebrum just anterior to the optic chiasm. Olfactory tract then divides into two branches which proceed towards the
temporal lobe of cerebrum. Temporal lobe of cerebrum contains the olfactory area which is responsible for the sense of olfaction.
- Optic nerve (second cranial)
It is
purely sensory nerve. The sensory receptors of the optic nerve are located in the
retina of the eye. The retina has two types of receptors:
Rods are responsible for black and white vision and
cons are responsible for color vision. Rods and cons then form synapses with
bipolar cells which synapse with ganglion cells.
Ganglion cells then converge to form optic nerve which leaves the eye and enters the
superior orbital fissure. From the superior orbital fissure it comes just below the anterior clinoid process. Here above the pituitary fossa the nerves form crossover called
optic chiasm. Fibers of the optic nerve on the medial side cross over to the opposite side at the optic chiasm and continue on the medial side of the other side. Fibers of the lateral side continue on the same side. Optic chiasm diverges posteriorly to form the
optic tracts. From the optic tract proceeds posteriorly and ends at the
medial and lateral geniculate nuclei located on both sides of the cerebral peduncles. Fibers from these nuclei proceeds further backwards and ends at the primary visual area located in the posterior part of the
occipital lobe.
- Oculomotor nerve (third cranial)

It arises from the
anterior surface of the med brain in between two cerebral peduncles. From the posterior cranial fossa it enters the lateral aspect of the petrous part of the temporal bone. Here it lies in a cave called
cavernus sinus. From the middle cranial fossa it passes into the orbit through the
superior orbital fissure. After emerging from the superior orbital fissure it divides into
upper and lower branches.
Upper branch innervates the
superior rectus muscle and levator palpebrii superioris muscle while the
lower branch innervates
inferior rectus, medial rectus and inferior oblique muscles. Along the lower fibers the
parasympathetic nerve fibers also enter which innervates the
ciliary muscle (causing accommodation of lens) and
sphincter papillae muscles (causing constriction of pupils).
- Trochlear nerve (fourth cranial)
It is the only cranial nerve arising from the
posterior surface of the mid brain. From the posterior cranial fossa it enters the lateral aspect of the petrous part of the temporal bone. Here it lies in a cave called
cavernus sinus. From the middle cranial fossa it passes into the orbit through the
superior orbital fissure. With in the orbit the Trochlear nerve innervates the only
superior oblique muscle.
- Trigeminal nerve (fifth cranial)
It arises from the
anterior side of the Pons. It proceeds from the posterior cranial fossa into the middle cranial fossa along the lateral side of the petrous part of the temporal bone. Here in the
cavernus cave the trigeminal nerve forms the
trigeminal ganglion. The trigeminal ganglion gives off
three branches of trigeminal nerve:
i. Ophthalmic nerve
ii. Maxillary nerve
iii. Mandibular nerve
Ophthalmic nerve (V1)
It passes from the middle cranial fossa through
superior orbital fissure. Below the roof of the orbit it gives off branches shown in the following figure.
Maxillary nerve (V2)
It arises from the trigeminal ganglion passes from the middle cranial fossa into infra temporal fossa through the
foramen rotundum. In the infra temporal fossa it divides into
two branches;
upper and lower branches.
Infra orbital nerve from the upper branch passes through a tunnel called
infra orbital groove in the floor of the orbit. It appears below the lower margin of the orbit and divides into
three cutaneous branches:
Palpebral supplying the lower eyelid
Nasal supplying lateral part of nose
Labial supplying upper lips
Anterior superior alveolar nerve of the
lower branch also passes through the
infra orbital groove along the infra orbital nerve and makes a turn posteriorly after emerging from the
infra orbital foramen. Posteriorly it joins the posterior superior alveolar nerve which appears here after passing through bony tunnels in the maxilla. They form a loop like structure from which gives the
superior dental and gingival nerves innervating the upper teeth and upper gums. Other branches of lower part of the maxillary nerve include
palatine nerves (greater and lesser palatine nerves) which innervate mucosa of the hard, soft palate and nasal mucosa.
Nasopalatine nerve innervates the nasal septum.
Zygomatic nerve is also a branch of lower part of maxillary nerve which divides into
frontal and temporal nerves innervating the skin over the cheek bones.
Mandibular nerve (V3)
It arises from the trigeminal ganglion in the cavernus sinus of the middle cranial fossa. From here it passes downwards and enters the infra temporal fossa through the
foramen ovale. Here it gives
sensory and
motor branches. Motor branches innervate the muscles of mastication, these are masseter, temporalis, medial and lateral pterygoid muscles.
Small motor branches innervate the tensor tympani and tensor veli palatine.
Sensory branches are
buccal nerve which innervates the cheeks (lateral part).
Auricotemporal nerve passes upwards behind the neck of the mandible and innervates the skin on the lateral side of the forehead. Two main terminal branches of the mandibular nerve are the inferior
alveolar nerve and lingual nerve.
Inferior alveolar is the posterior branch which passes through the
mandibular foramen in the mandible then continues in the mandible through the
mandibular canal. While passing through the mandibular canal it gives off
inferior dental and gingival nerves which innervate the lower teeth and lower gums. The terminal part of the inferior alveolar nerve emerges from the mandible through the
mental foramen. As it emerges from the mental foramen it is called
mental nerve which innervates the skin of the chin on the corresponding ipsilateral area. Before entering the mandibular foramen a small nerve called
myohoid nerve separate from it and innervates the myolohoid muscle and anterior belly of digastrics muscle.
Lingual nerve passes in front of inferior alveolar nerve and passes downward between the lateral surface of medial pterygoid muscle and medial surface of the mandible. At its origin it receives branches from seventh cranial nerve (facial nerve) called
chorda tympani. Chorda tympani and lingual nerve passes downward jointly and innervates the anterior two third of the tongue responsible for taste (chorda tympani) and general sensation from anterior two third of the tongue (lingual nerve).
- Abducent nerve (sixth cranial)
This nerve arises in between the
Pons and Medulla oblongata. From the posterior cranial fossa it enters the lateral aspect of the petrous part of the temporal bone. Here it lies in a cave called
cavernus sinus. From the middle cranial fossa it passes into the orbit through the
superior orbital fissure. Within the orbit the Abducent nerve innervates the only
lateral rectus muscle.





 12:24 AM
12:24 AM
 Aftab Ahmad Khan Yousafzai
Aftab Ahmad Khan Yousafzai